The fluorescent lights of the emergency department at Metropolitan General Hospital buzzed overhead as nurses rushed to prepare a life-saving blood transfusion. It was supposed to be a straightforward procedure. A 32-year-old transgender woman named Morgan Ellis had been brought in after complications from a serious accident left her critically low on blood. Doctors had already cross-matched a compatible unit. The blood was ready. Then everything changed.

According to multiple witnesses inside the ward that evening, Morgan became visibly distressed when staff began preparing the transfusion. She reportedly asked pointed questions about the donor. When she learned the compatible blood had come from a male donor described as straight, she refused outright. Her voice rose as she declared, “I will not let Straight Man’s blood flow in my body.”
The room froze. Nurses paused mid-motion. One staff member tried to explain that blood donations are anonymous, rigorously screened for safety, and matched only by blood type and compatibility factors — not by the donor’s personal life, orientation, or identity. Morgan was unmoved. She repeated her refusal, framing the issue as a matter of personal boundaries and identity. What should have been a quiet medical moment turned into a loud, public argument that quickly pulled in more staff and nearby patients.
Word spread fast down the hallway. A charge nurse stepped in to de-escalate, but the tension only grew. Morgan insisted she could not accept the blood on principle. Staff emphasized the medical urgency — without the transfusion her condition could deteriorate rapidly. She pushed back, arguing that her sense of self would not allow it. Voices overlapped. A patient in a nearby bed sat up to watch. Another visitor pulled out a phone. The confrontation was no longer private.
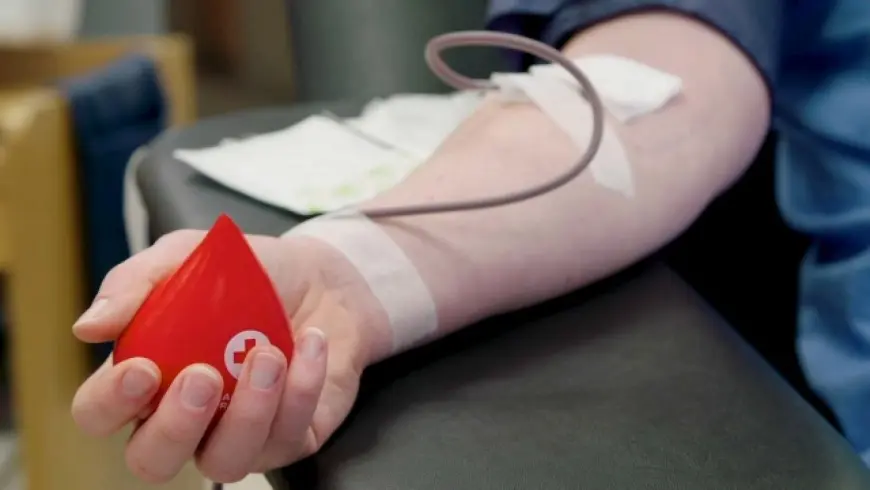
Hospital leadership was alerted immediately. The director of the medical center, Dr. Elena Vargas, arrived within minutes and took charge of the situation. She spoke calmly but firmly, attempting to separate medical facts from the growing emotional storm. Dr. Vargas explained that blood banks do not categorize or label units according to a donor’s sexual orientation or gender identity. Every unit goes through the same strict testing process for infectious diseases, antibodies, and compatibility. The donor’s private life has no bearing on the safety or effectiveness of the transfusion for the recipient.
Morgan reportedly stood her ground. She repeated that she would not allow “Straight Man’s blood” inside her. The director listened, then reiterated the hospital’s duty to provide evidence-based care while respecting patient autonomy where possible. She offered to explore alternatives, though in emergency transfusion scenarios options are often limited to what is already cross-matched and available. The discussion circled the same core tension: one side grounded in clinical reality and anonymous donation protocols, the other rooted in the patient’s stated personal and ideological boundaries.

By now the area had become a scene of open uproar. Staff members exchanged glances. Some appeared stunned, others tried to maintain professionalism while managing the growing crowd of onlookers. A few patients and family members whispered among themselves. One person allegedly filmed part of the exchange before being asked to stop. The air felt thick with discomfort and disbelief. What began as a medical necessity had become a flashpoint that exposed raw divisions over identity, medicine, and where personal beliefs end and life-saving treatment begins.
Dr. Vargas continued trying to bridge the gap. She acknowledged that patients have the right to refuse treatment, even when doctors strongly recommend it. At the same time, she stressed that the blood supply system is deliberately designed to remove personal details from the equation precisely so that anyone in need can receive help without ideological filters. The screening process focuses on behavior-based risk factors and laboratory testing, not on labeling donors as “straight,” “gay,” or any other identity category.
Introducing such distinctions at the point of transfusion, she noted, would upend the entire anonymous donation model that hospitals rely on.
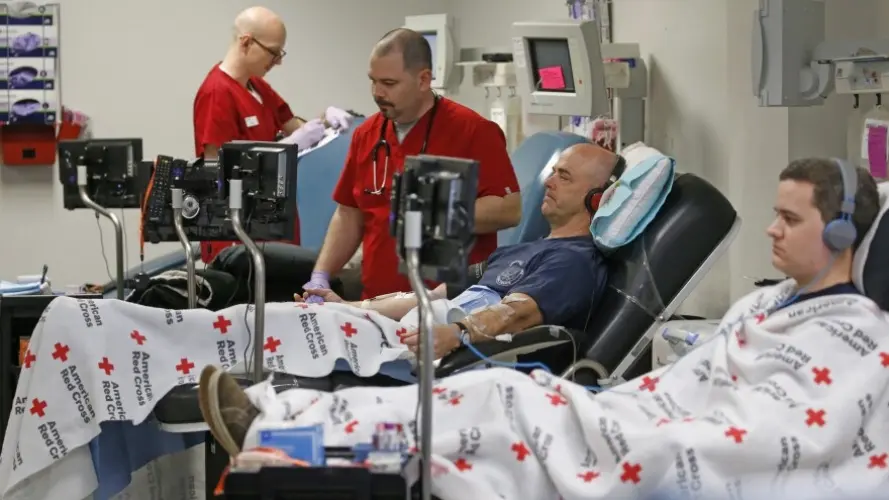
Morgan’s refusal created an immediate practical problem. The hospital could not force the transfusion. Staff explored whether another compatible unit from a different donor could be located quickly, though in many facilities inventory is tightly managed and alternatives are not always instantly available. Time pressure mounted. Nurses monitored vital signs while administrators weighed legal and ethical obligations. Patient autonomy is a cornerstone of modern medicine, yet so is the duty to provide care without unnecessary delay when someone’s life hangs in the balance.
The confrontation eventually drew attention beyond the immediate ward. Whispers of the incident spread through the hospital and, according to later reports, began appearing on social media. Some online reactions framed it as a troubling example of identity politics overriding medical reality. Others defended the patient’s right to set personal boundaries, even in crisis. The story, still unfolding in real time for those present, quickly took on a life of its own as people debated the proper limits of personal belief when blood and biology are involved.
Inside the hospital, Dr. Vargas and her team continued working to find a path forward. They reiterated offers of information, alternative explanations, and support. Morgan remained firm in her position. The standoff highlighted a collision between two frameworks: one that treats blood as a standardized, tested biological product stripped of the donor’s personal story, and another that views any medical intervention through the lens of identity and symbolic meaning. For the medical staff caught in the middle, the priority remained stabilizing the patient while navigating an unexpected minefield of personal conviction.

Hours later the situation had not fully resolved. Hospital officials declined to comment on specific patient details, citing privacy rules. Witnesses described a charged atmosphere that lingered long after the initial argument. Some staff expressed concern that such incidents could erode trust in the blood donation system if people began demanding donor information that is intentionally kept private. Others worried about the precedent of allowing non-medical criteria to influence emergency care decisions.
The episode at Metropolitan General Hospital has since sparked wider conversation about the intersection of personal identity, medical ethics, and the practical realities of emergency transfusion medicine. Blood donation relies on millions of anonymous contributors whose only shared trait is the willingness to give. The system works because compatibility is determined in the lab, not in personal interviews or ideological checklists. When that boundary is challenged in a moment of crisis, the results can be as dramatic as they are divisive.
For Morgan Ellis, the night became a public test of principle versus physiology. For the hospital staff and director who intervened, it became a stark reminder that even the most routine medical procedures can explode into larger cultural conflicts when identity claims meet biological necessity. And for the onlookers who watched the confrontation unfold, it left a lingering question: in a life-or-death moment, how much weight should personal narrative carry against the cold, screened reality of donated blood?
The answers remain unsettled. What is clear is that one hospital corridor witnessed a collision few expected — and many will continue debating long after the fluorescent lights dimmed.





